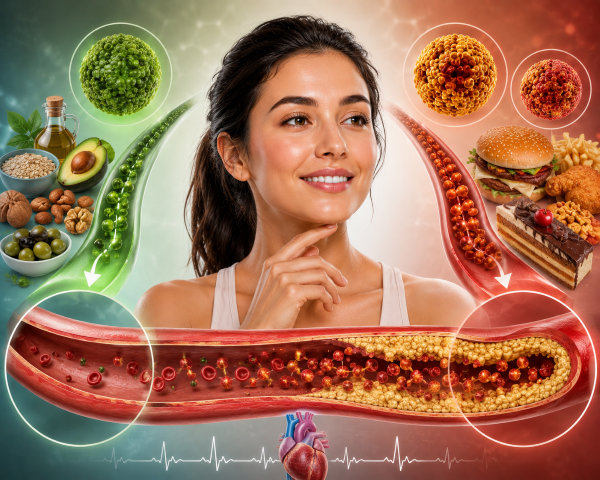
What Is Cholesterol?
Cholesterol is a waxy, fat-like substance produced by the liver and found in every cell of the body. It is essential for building cell membranes, producing hormones (including oestrogen, testosterone and cortisol), synthesising vitamin D, and making bile acids needed for digestion. The problem is not cholesterol itself — it is when certain types accumulate in excessive amounts in the bloodstream.
The Three Key Numbers
LDL — Low-Density Lipoprotein ("Bad" Cholesterol)
LDL carries cholesterol from the liver to cells throughout the body. When there is more LDL than cells can use, the excess circulates in the blood and can deposit inside artery walls, forming plaques. Over time these plaques narrow and harden arteries — a process called atherosclerosis — raising the risk of heart attack and stroke.
Target: Below 100 mg/dL for most adults; below 70 mg/dL for those at high cardiovascular risk.
HDL — High-Density Lipoprotein ("Good" Cholesterol)
HDL acts as a rubbish collector, picking up excess cholesterol from the bloodstream and arterial walls and returning it to the liver for disposal. Higher HDL levels are strongly protective against heart disease.
Target: Above 60 mg/dL is considered protective. Below 40 mg/dL (men) or 50 mg/dL (women) is a risk factor.
Triglycerides
Triglycerides are the most common type of fat in the body. They store unused calories and are elevated by excess sugar, refined carbohydrates, and alcohol. High triglycerides combined with low HDL is particularly dangerous.
Target: Below 150 mg/dL. Above 200 mg/dL is borderline high.
What Raises LDL Cholesterol?
- Saturated and trans fats — found in fatty meats, full-fat dairy, palm oil, and processed snacks
- Excess dietary cholesterol — particularly from organ meats and processed meats
- Physical inactivity — exercise raises HDL and improves LDL particle size
- Obesity — especially visceral (abdominal) fat raises LDL and triglycerides
- Genetics — familial hypercholesterolaemia affects 1 in 250 people and causes very high LDL regardless of diet
- Hypothyroidism and diabetes — both raise LDL independently
Evidence-Based Ways to Improve Your Cholesterol Profile
Eat More Soluble Fibre
Soluble fibre binds LDL cholesterol in the digestive tract and removes it before it enters the bloodstream. Oats, barley, lentils, kidney beans, psyllium husk, apples, and flaxseed are the most effective sources. Adding 5–10g of soluble fibre daily lowers LDL by approximately 5%.
Replace Saturated Fat With Unsaturated Fat
Swapping butter for olive oil, choosing fatty fish over red meat, and eating nuts and avocado — all of which are rich in monounsaturated and polyunsaturated fats — reduces LDL and raises HDL simultaneously.
Exercise Regularly
Aerobic exercise (brisk walking, jogging, cycling) for at least 150 minutes per week raises HDL by 5–10% and modestly reduces LDL. Resistance training adds further benefit.
Lose Excess Weight
Losing just 5–10% of body weight can lower LDL by 5–8% and reduce triglycerides significantly.
Limit Alcohol and Sugar
Both raise triglycerides. Cutting added sugar and reducing alcohol to moderate levels has a rapid effect on triglyceride levels — often within weeks.
When Medication Is Needed
For people with genetically high cholesterol, established heart disease, or persistently elevated LDL despite lifestyle changes, statins are among the most well-studied and effective medications in medicine. They reduce the risk of heart attack and stroke by 25–35%. The decision to start medication should always be made with a doctor based on your full cardiovascular risk profile — not just one number.
The Takeaway
Get a fasting lipid panel (blood test) as part of your annual health check. Knowing your HDL, LDL, and triglycerides gives you a clear picture and allows targeted action well before any symptoms appear.